PLUM / Claims / System Design
Helping first-time claimants file reimbursements effortlessly
Replaced manual claim filing with a guided product workflow that enabled self-service submissions and reduced operational effort.
/ About Plum
A digital health insurance platform helping companies manage employee healthcare and insurance benefits. Expanding their footprints in primary healthcare & wellness and B2C space.
/ Context
There are three types of insurance claims
Emergency
Planned treatment
Reimbursements
Emergency and planned treatments are cashless claims. Reimbursements formed more than 45% of overall claims and required users to submit documents after treatment to receive payment. We observed many users struggling to complete reimbursements.
/ problem
Filing a claim is a high-anxiety moment of truth, but our process was making it harder, with 30-day timelines, constant back-and-forth, and Claims NPS of 29.
/ pain points
Unclear requirements
Confusion around documents
Repeated corrections after submission
Dependency on the support team
Manual verification effort
Long submission delays
/ Why this problem was critical to solve
For many employees, reimbursement is the first time they truly experience how insurance works. When users could not complete claims correctly, they depended on support, and operations had to fix submissions manually. This increased processing time and operational cost, and reduced confidence in the product. To scale insurance digitally, the product needed to guide users through the process before submission, not correct it after.
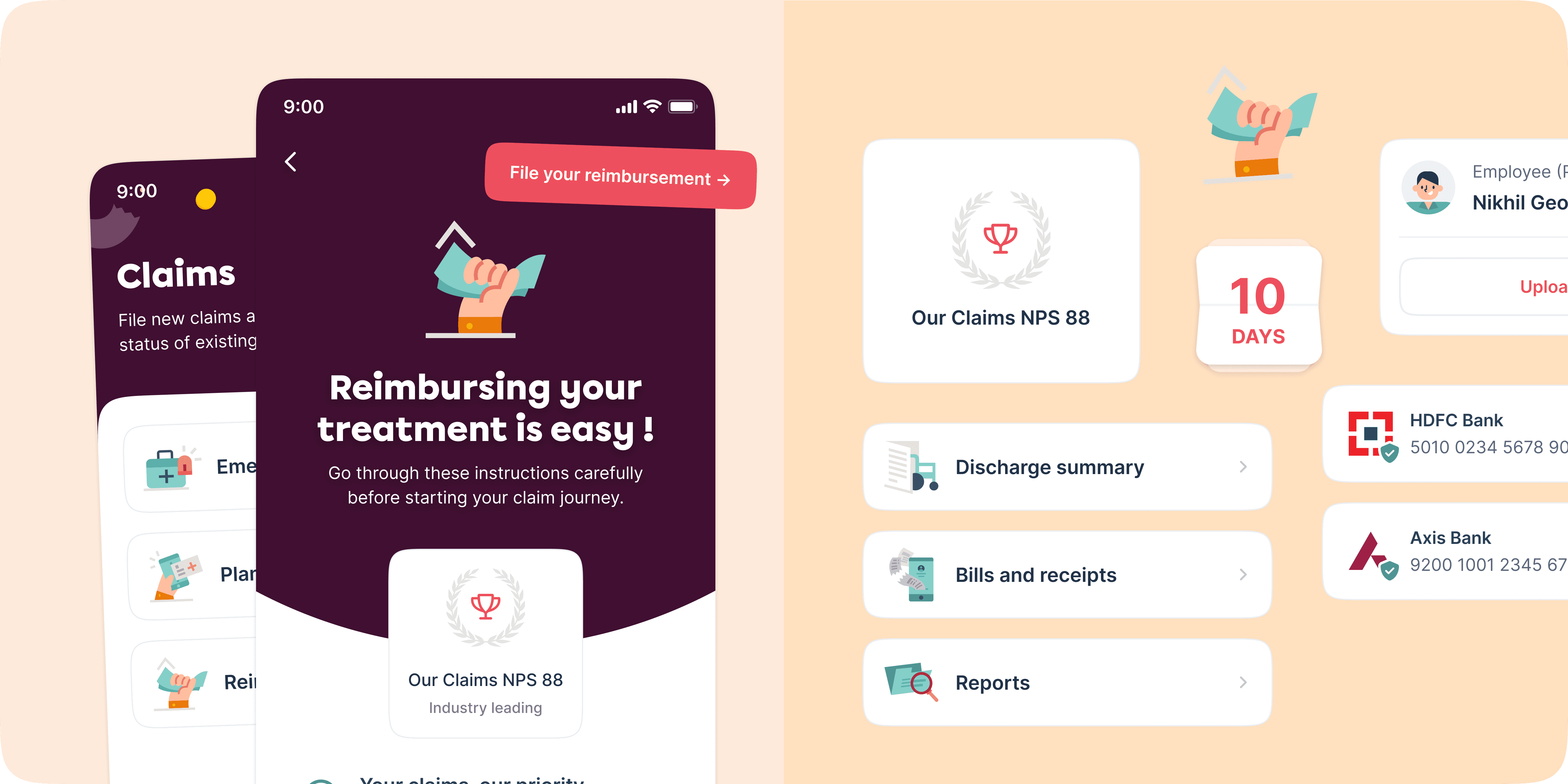
/ Final Designs
Instead of forcing users to adapt to insurer workflows, we redesigned the experience to work for them. We transformed the claims into a step by step journey: Digitising forms, providing real time guidance, and building confidence at every touch point.
/ Final design
Interactive prototype